Why USA Mental Health Practices Are Turning to a Mental Health Billing Services Company for Faster Reimbursements
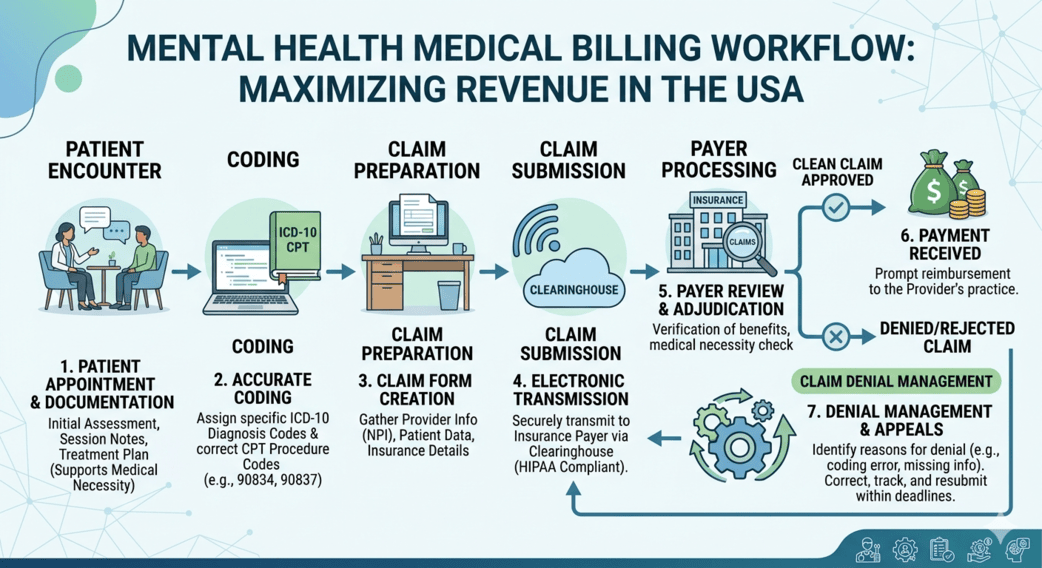
Introduction
Mental health providers across the USA are facing growing administrative pressure. Between changing payer guidelines, evolving CPT codes, increasing claim denials, and stricter documentation standards, managing billing internally has become more complicated than ever. Therapists, psychologists, psychiatrists, counselors, and behavioral health clinics are now spending valuable clinical time handling insurance paperwork instead of focusing on patient care.
That shift is one of the biggest reasons healthcare organizations are partnering with a reliable mental health billing services company. From improving reimbursement accuracy to reducing denied claims, specialized billing support helps practices maintain financial stability while enhancing operational efficiency.
Unlike general billing providers, companies focused on behavioral health understand the unique challenges of mental health insurance billing. They know how to navigate psychotherapy coding, telehealth regulations, authorization requirements, payer-specific rules, and compliance standards that directly affect behavioral health reimbursement.
In today’s competitive healthcare environment, having a specialized billing partner is no longer just an operational convenience — it has become a strategic advantage.
The Growing Complexity of Mental Health Insurance Billing in the USA
Mental health billing is very different from traditional medical billing. Behavioral health claims often involve:
- Time-based CPT coding
- Frequent modifier usage
- Pre-authorizations
- Telehealth compliance
- Documentation audits
- Payer-specific therapy limitations
- Coordination of benefits
Even experienced office staff can struggle to keep up with these constantly changing requirements.
A single coding error or missing modifier can delay reimbursement for weeks. In some cases, repeated claim mistakes may trigger payer audits or increased scrutiny from insurance companies.
This is why many clinics now depend on mental health insurance billing services to manage the entire reimbursement process more efficiently.
What Does a Mental Health Billing Services Company Actually Do?
A professional mental health billing services agency handles the financial side of behavioral healthcare practices. Their role extends beyond simply submitting claims.
Most companies provide:
Insurance Verification
Before appointments, billing teams verify:
- Coverage eligibility
- Copays
- Deductibles
- Prior authorization requirements
- Out-of-network benefits
This reduces front-end claim issues and improves patient transparency.
Accurate Coding Support
A qualified mental health billing specialist ensures claims use the correct:
- CPT codes
- ICD-10 diagnosis codes
- Modifiers
- Telehealth indicators
Behavioral health coding errors are one of the leading causes of delayed payments.
Claim Submission and Tracking
An experienced mental health billing provider electronically submits claims, tracks payer responses, and follows up on unpaid balances.
Instead of waiting months for reimbursements, practices receive faster payment cycles and fewer denials.
Denial Management
One major advantage of working with a mental health billing consultant is proactive denial management.
Specialists identify recurring problems such as:
- Incomplete documentation
- Authorization issues
- Duplicate claims
- Invalid diagnosis combinations
- Credentialing mismatches
Correcting these patterns significantly improves revenue performance.
Why More Practices Outsource Mental Health Billing Services
Behavioral health organizations are increasingly choosing to outsource mental health billing services instead of hiring large in-house teams.
The reason is simple: outsourcing reduces administrative stress while improving collections.
Lower Operational Costs
Maintaining an internal billing department can be expensive. Practices must pay for:
- Staff salaries
- Training
- Software
- Compliance updates
- Employee turnover
- Technology upgrades
With outsourced mental health billing, providers gain access to experienced billing professionals without carrying the full cost of an in-house team.
Better Revenue Performance
The best mental health billing agency focuses heavily on clean claims and timely submissions.
This leads to:
- Reduced denials
- Improved cash flow
- Faster reimbursements
- Better aging management
- Increased collections
Many behavioral health clinics notice measurable revenue improvements within a few months of outsourcing.
Reduced Administrative Burnout
Mental health professionals already deal with emotionally demanding workloads. Administrative overload only adds more stress.
By using billing services for mental health therapists, providers can focus more on patient outcomes rather than payer disputes and claim follow-ups.
Key Features of the Best Mental Health Billing Agency
Not every billing partner understands behavioral health complexities. Choosing the right company matters.
Here are some qualities to look for when evaluating a professional mental health billing company.
Behavioral Health Expertise
A specialized company should understand:
- Psychiatry billing
- Psychotherapy CPT codes
- Group therapy billing
- Substance abuse billing
- Telepsychiatry claims
- Insurance regulations for behavioral health
Experience in general medical billing alone is not enough.
Transparent Reporting
The best outsource mental health billing and coding company provides detailed financial reports including:
- Claim status updates
- Collection rates
- Denial trends
- Accounts receivable reports
- Revenue analytics
Clear reporting helps practices make informed financial decisions.
HIPAA Compliance
Patient privacy remains critical in behavioral healthcare.
Reliable mental health billing companies use secure systems and maintain strict HIPAA compliance protocols to protect sensitive patient data.
Scalable Support
As practices grow, billing needs become more complex.
An experienced mental health billing agency should be able to support:
- Multi-location practices
- Expanding provider teams
- Telehealth growth
- New payer enrollments
- High-volume claim processing
Common Billing Challenges Mental Health Providers Face
Many behavioral health clinics underestimate how small billing problems can affect long-term revenue.
Here are some of the most common issues providers encounter.
Frequent Claim Denials
Behavioral health claims are often denied due to:
- Missing authorizations
- Incorrect modifiers
- Time-based coding errors
- Documentation deficiencies
Professional mental health medical billing services help reduce these issues significantly.
Delayed Insurance Payments
Slow payer reimbursements can disrupt cash flow and impact practice operations.
An experienced team handling mental health insurance billing actively follows up with insurers to minimize delays.
Credentialing Problems
Claims may be rejected if providers are not properly credentialed with insurance networks.
Many billing firms now combine billing support with credentialing services to streamline payer enrollment and avoid unnecessary claim rejections.
Telehealth Billing Confusion
Telehealth usage expanded rapidly across the USA, but payer rules continue to change frequently.
A modern mental health medical billing solution keeps practices updated on evolving telehealth billing requirements and reimbursement guidelines.
The Role of Medical Coding in Behavioral Health Revenue
Coding accuracy directly affects reimbursement success.
Incorrect diagnosis coding can trigger denials, compliance risks, or underpayments. That is why many practices seek integrated medical coding services alongside billing support.
Behavioral health coding requires attention to:
- Medical necessity
- Session duration
- Diagnosis specificity
- Documentation alignment
- Payer-specific policies
An experienced mental health billing and coding company ensures coding accuracy while reducing compliance risks.
Why Revenue Cycle Management Matters for Mental Health Practices
Billing is only one part of financial performance.
Comprehensive revenue cycle management services help practices optimize the entire reimbursement lifecycle, including:
- Patient scheduling
- Eligibility verification
- Claim creation
- Payment posting
- Denial appeals
- Patient collections
- Financial reporting
For behavioral health providers, effective revenue cycle management improves both operational efficiency and long-term profitability.
A strong RCM strategy also helps practices prepare for changing insurance regulations and evolving reimbursement models across the USA healthcare system.
Real-World Example: How Outsourcing Improved a Behavioral Health Clinic
A mid-sized behavioral health clinic in Texas struggled with rising denials and delayed payments after expanding telehealth services.
Their internal staff had difficulty managing:
- Multiple insurance plans
- Telehealth modifiers
- Authorization tracking
- Aging claims
After partnering with a top outsource mental health billing company, the clinic achieved:
- Faster reimbursement turnaround
- Reduced denial rates
- Improved claim accuracy
- Better patient billing communication
- Stronger monthly cash flow
Most importantly, providers spent less time dealing with administrative issues and more time supporting patients.
How to Choose the Right Mental Health Billing Provider
Selecting the right billing partner should involve more than comparing prices.
Here are a few practical questions practices should ask before hiring a billing company.
Do They Specialize in Behavioral Health?
A company focused specifically on mental health medical billing services outsourcing will better understand industry-specific challenges.
What Is Their Denial Rate?
Low denial rates often indicate stronger claim quality and payer expertise.
Do They Offer Credentialing Support?
Integrated credentialing services can simplify payer enrollment and reduce claim delays.
Can They Handle Scaling?
Your billing partner should support practice growth without sacrificing claim quality or communication.
Do They Provide Dedicated Support?
Working with a responsive account manager or mental health billing specialist improves issue resolution and communication.
The Future of Mental Health Billing in the USA
Behavioral healthcare demand continues to rise across the USA. At the same time, insurance regulations, telehealth expansion, and payer scrutiny are increasing billing complexity.
As practices grow, many providers are moving toward:
- Automation-driven billing workflows
- AI-assisted coding review
- Outsourced RCM support
- Integrated patient payment systems
- Specialized behavioral health billing partnerships
The demand for reliable billing services for mental health providers will continue growing as clinics seek greater financial stability and operational efficiency.
Supporting Long-Term Growth with Specialized Billing Solutions
Modern healthcare practices need more than simple claim submission support. They need strategic financial guidance and operational efficiency.
That is why many organizations now partner with companies offering:
- medical billing services
- medical coding services
- medical billing and coding services
- revenue cycle management services
- credentialing services
Behavioral health clinics especially benefit from integrated solutions that combine compliance expertise, payer knowledge, and scalable billing support.
Companies like 247 Medical Billing Services help practices navigate the growing complexity of behavioral healthcare reimbursement while improving revenue performance in a highly competitive healthcare landscape.
Conclusion
Managing behavioral health reimbursements has become increasingly challenging for providers across the USA. Insurance complexities, coding requirements, authorization rules, and telehealth regulations continue to evolve rapidly.
Partnering with a trusted mental health billing services company allows practices to reduce administrative burdens, improve claim accuracy, and strengthen financial performance without sacrificing patient care quality.
Whether a clinic needs a full mental health medical billing solution, coding expertise, denial management, or complete outsourced mental health billing, specialized support can make a measurable difference in both operational efficiency and revenue growth.
As the healthcare industry continues changing, behavioral health providers who invest in professional billing support will be better positioned for sustainable long-term success.
FAQs
What does a mental health billing services company do?
A mental health billing services company manages insurance verification, coding, claim submission, denial management, payment posting, and reimbursement follow-up specifically for behavioral health providers.
Why should practices outsource mental health billing services?
Practices often outsource to reduce administrative workload, improve claim accuracy, lower denial rates, and increase reimbursement efficiency while focusing more on patient care.
How is mental health billing different from general medical billing?
Mental health billing involves time-based CPT codes, therapy modifiers, telehealth regulations, authorization requirements, and behavioral health-specific insurance policies that require specialized expertise.
What should providers look for in a mental health billing agency?
Providers should evaluate industry experience, HIPAA compliance, denial management performance, reporting transparency, credentialing support, and behavioral health specialization.
Do mental health billing companies help with credentialing?
Many companies offer integrated credentialing services to help providers enroll with insurance networks and reduce claim rejections caused by payer enrollment issues.
Can outsourced mental health billing improve revenue?
Yes. Experienced billing specialists often improve reimbursement speed, reduce denials, optimize coding accuracy, and strengthen overall revenue cycle performance for behavioral health practices